Machine learning-predicted insulin resistance was related to the next threat of diabetes, heart problems, and mortality within the UK Biobank
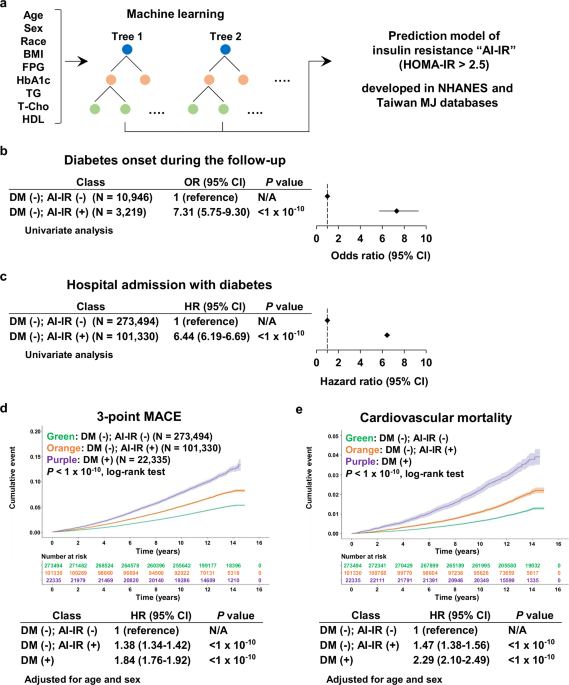
To guage the predictive functionality of AI-IR (Fig. 1a) for the incidence of diabetes, heart problems, and mortality within the UK Biobank, we first appeared on the impact of AI-IR on the incidence of diabetes amongst individuals with out diabetes at baseline and accomplished follow-up go to (N = 14,165, baseline traits are proven in Supplementary Desk 1). Throughout a imply follow-up of 4.28 years (95% confidence interval [CI], 3.41–5.15), 309 individuals (2.18%) developed diabetes. AI-IR constructive individuals had a considerably increased threat of creating diabetes in comparison with AI-IR damaging individuals (odds ratio [OR], 7.31; 95% CI, 5.75–9.30; P < 1 × 10−10, Fig. 1b). Notably, though AI-IR was initially developed utilizing fasting blood take a look at outcomes, blood samples within the UK Biobank weren’t constantly collected within the fasted state. To deal with this, we stratified individuals into three teams primarily based on fasting length previous to blood assortment (lower than 4 h, 4 or extra and fewer than 8 h, 8 h or extra) and examined the affiliation between AI-IR and the incidence of diabetes. Throughout all classes, AI-IR constructive individuals constantly confirmed a considerably increased threat of creating diabetes, supporting the robustness of our mannequin (Supplementary Fig. 1a–c). Hereafter, to keep up most pattern dimension, we didn’t stratify or exclude individuals primarily based on fasting length. In a complementary evaluation leveraging the Nationwide Well being Service (NHS) medical document system, we appeared on the impact of AI-IR on hospital admission with diabetes amongst individuals with out diabetes at baseline (Baseline traits of individuals are proven in Supplementary Desk 2). AI-IR constructive individuals had a markedly increased threat of admission with diabetes (hazard ratio [HR], 6.44; 95% CI, 6.19–6.69; P < 1 × 10−10, Fig. 1c). Of notice, AI-IR was related to a considerably increased threat of diabetes onset and hospital admission with diabetes after adjusting for age and intercourse, and even after adjusting for age, intercourse, and BMI, indicating that our machine learning-based prediction mannequin is ready to seize a BMI-independent impact of insulin resistance (Supplementary Fig. 2a, b).
a A diagram depicting the development of a machine studying mannequin to foretell insulin resistance (HOMA-IR > 2.5) that makes use of 9 medical parameters. b Impact of AI-IR on the percentages ratio (OR) for onset of diabetes throughout the follow-up interval in individuals with out diabetes (DM) at baseline. Logistic regression was used with a two-sided Wald take a look at. Within the graph, factors signify the estimated OR, and error bars signify 95% confidence intervals. c Impact of AI-IR on the hazard ratio (HR) for hospital admission as a result of diabetes in individuals with out DM at baseline. Cox proportional hazards mannequin was used with a two-sided Wald take a look at. Within the graph, factors signify the estimated HR, and error bars signify 95% confidence intervals. d, e Kaplan–Meier plot for cumulative incidence of 3-point MACE (d) or cardiovascular mortality (e) in DM (-); AI-IR (-), DM(-); AI-IR (+), and DM (+) group. Within the graph, the strains signify the estimated cumulative incidence, and the shaded error bands signify 95% confidence intervals. The HRs adjusted for age and intercourse are additionally proven for 3-point MACE (d) and cardiovascular mortality (e). Cox proportional hazards mannequin was used with a two-sided Wald take a look at. Supply information are supplied as a Supply information file.
Heart problems is a significant complication of insulin resistance and diabetes. Due to this fact, we additionally appeared on the impact of AI-IR on 3- and 4-point main opposed cardiovascular occasion (MACE). Results on cardiovascular mortality and general mortality have been additionally examined. Baseline traits of individuals are proven in Supplementary Desk 2. As anticipated, a Kaplan-Meier plot revealed a big distinction within the cumulative incidence of 3-point MACE between individuals with diabetes, these with out diabetes however constructive for AI-IR, and people with out diabetes and damaging for AI-IR (Fig. 1d, log-rank take a look at P < 1 × 10−10). The HR adjusted for age and intercourse was highest in individuals with diabetes (HR, 1.84; 95% CI, 1.76-1.92; P < 1 × 10−10), adopted by these with out diabetes however constructive for AI-IR (HR, 1.38; 95% CI, 1.34–1.42; P < 1 × 10−10), after which these with out diabetes and damaging for AI-IR (Fig. 1d). AI-IR and diabetes was considerably related to the next threat of 3-point MACE even after adjusting for age, intercourse, and BMI (Supplementary Fig. 2c). We additionally noticed that AI-IR was considerably related to an elevated threat of 4-point MACE, cardiovascular mortality, and general mortality (Fig. 1e and Supplementary Fig. second–f).
Machine learning-predicted insulin resistance permits improved diabetes threat stratification in comparison with beforehand reported metrics
To look at whether or not AI-IR outperforms beforehand established easier metrics of weight problems, metabolic syndrome, and insulin resistance, we in contrast the predictive capabilities of AI-IR, BMI, metabolic syndrome (MetS), TG/HDL ratio, and TyG index for the incidence of diabetes amongst people with out diabetes at baseline throughout the follow-up interval. TG/HDL ratio24,25 and TyG index26,27,28 has been reported as surrogate markers of insulin resistance. Space below the curve (AUC) of the receiver working attribute (ROC) curve was highest for AI-IR (0.798, P < 1 × 10−4 vs different metrics), adopted by MetS (0.748), BMI (0.721), TyG index (0.703), and TG/HDL ratio (0.702), indicating the AI-IR demonstrated the very best predictive efficiency amongst these metrics (Fig. 2a). Subsequent, we categorized people with out diabetes at baseline into 4 teams in response to each AI-IR standing (constructive or damaging) and their standing on beforehand established metrics (constructive or damaging). BMI of 30, TG/HDL ratio of three.025, and TyG index of 4.6827 have been used as cut-off values in response to earlier literatures. After we categorized people into 4 teams primarily based on AI-IR standing (constructive or damaging) and BMI ( ≥ 30 or <30), we noticed that the incidence of diabetes was considerably increased (P = 2.52 × 10−5) within the AI-IR single-positive group (OR, 6.14; 95% CI, 4.42–8.54; P < 1 × 10−20; adjusted for age and intercourse) in contrast with the BMI single-positive group (OR, 0.86; 95% CI, 0.35–2.12; P = 0.74). Of notice, a BMI of 30 or increased alone didn’t considerably enhance diabetes incidence when people have been damaging for AI-IR, suggesting that these topics could signify a metabolically wholesome weight problems phenotype. In distinction, diabetes incidence was markedly increased (P = 9.78 × 10−7) within the AI-IR and BMI double-positive group (OR, 8.08; 95% CI 6.13–10.66; P < 1 × 10−20) in contrast with the BMI single constructive group, underscoring that AI-IR gives considerably improved diabetes threat stratification amongst people with weight problems (BMI ≥ 30; Fig. 2b). Equally, after we categorized people with out diabetes into 4 teams primarily based on each AI-IR standing (constructive or damaging) and MetS (constructive or damaging), the incidence of diabetes was considerably increased (P = 1.55 × 10−3) within the AI-IR single-positive group (OR, 6.85; 95% CI, 4.35–10.80; P = 1.2 × 10−16) in contrast with the MetS single-positive group (OR, 3.14; 95% CI, 2.07–4.77; P = 6.8 × 10−8). Once more, the incidence of diabetes was even better (P = 2.19 × 10−13) within the AI-IR and MetS double-positive group (OR, 11.71; 95% CI 8.53–16.06; P < 1 × 10−20) in contrast with the MetS single-positive group (Fig. 2c). We noticed the identical sample for TG/HDL ratio and TyG index (Fig. second, e). Collectively, these outcomes indicated that AI-IR was considerably related to the next threat of diabetes, heart problems, and mortality within the UK Biobank inhabitants. Furthermore, AI-IR demonstrated the very best predictive functionality for the incidence of diabetes in comparison with beforehand established metrics, offering the rationale for investigating the affiliation between predicted insulin resistance and most cancers incidence in subsequent analyses.

a Receiver working attribute (ROC) curve illustrating the predictive efficiency of AI-IR, BMI, Metabolic Syndrome, TG/HDL ratio, and TyG index for the incidence of diabetes throughout the follow-up interval. The realm below the curve (AUC) for every metrics can be proven. b–e Impact of AI-IR and BMI (b), Metabolic syndrome (MetS) (c), TG/HDL ratio (d), or TyG index (e) on the percentages ratio (OR) for onset of diabetes throughout the follow-up interval in individuals with out diabetes at baseline, adjusted for age and intercourse. Logistic regression was used with a two-sided Wald take a look at. Within the graph, factors signify the estimated OR, and error bars signify 95% confidence intervals. Supply information are supplied as a Supply information file.
Impact of machine learning-predicted insulin resistance on the incidence of most cancers
To analyze the impact of AI-IR on the incidence of most cancers, we leveraged the linkage between the UK Biobank and the NHS medical document system and examined the incidence of most cancers amongst individuals who have been cancer-free on the baseline go to (N = 372,395). We in contrast individuals with out diabetes and damaging for AI-IR (N = 256,685), these with out diabetes however constructive for AI-IR (N = 94,782), and people with diabetes (N = 20,928). Of 372,395 individuals who have been cancer-free at baseline, 51,193 developed most cancers (Supplementary Desk 3). After we merged all forms of most cancers, we didn’t observe any variations in most cancers incidence between the three teams. The HR adjusted for age and intercourse in individuals with out diabetes however constructive for AI-IR was 1.012 (95% CI, 0.992–1.033; P = 0.228), and that in individuals with diabetes was 0.973 (95% CI, 0.938–1.008; P = 0.129) (Fig. 3 and Supplementary Desk 4). Nevertheless, after we checked out particular person forms of most cancers, each AI-IR and diabetes have been related to a considerably increased threat of incidence of a number of most cancers varieties (The outcomes of the 25 frequent cancers are proven in Fig. 3, and the whole checklist will be present in Supplementary Desk 4). We examined the incidence of 36 cancers frequent to each women and men, 4 most cancers varieties particular to males, and three most cancers varieties particular to females. The Bonferroni-corrected P worth for significance was 0.05/43 = 1.163 × 10−3. The impact of AI-IR on growing the danger of the incidence was strongest for uterine most cancers (HR; 2.340; 95% CI, 2.065-2.652; P = 1.00 × 10−9), adopted by kidney most cancers (HR, 1.557; 95% CI, 1.367–1.772; P = 1.00 × 10−9) and esophagus most cancers (HR, 1.464; 95% CI, 1.253–1.710; P = 1.61 × 10−6). It was additionally related to the next incidence of renal pelvis most cancers (HR, 1.417; 95% CI, 1.013–1.983; P = 0.0418), small gut most cancers (HR, 1.393; 95% CI, 1.019–1.905; P = 0.0376), abdomen most cancers (HR, 1.374; 95% CI, 1.132–1.667; P = 1.28 × 10−3), liver and gallbladder (GB) most cancers (HR, 1.367; 95% CI, 1.114–1.678; P = 2.73 × 10−3), pancreas most cancers (HR, 1.291; 95% CI, 1.117–1.492; P = 5.58 × 10−4), colon most cancers (HR, 1.176; 95% CI, 1.084–1.276; P = 9.45 × 10−5), leukemia (HR, 1.164; 95% CI, 1.012–1.339; P = 0.0337), bronchial and lung most cancers (HR, 1.136; 95% CI, 1.048–1.231; P = 2.02 × 10−3), and breast most cancers (HR, 1.135; 95% CI, 1.075–1.199; P = 5.92 × 10−6). After we thought of the Bonferroni correction, AI-IR was related to the next incidence of uterine, kidney, esophagus, pancreas, colon, and breast cancers. However, AI-IR was related to a considerably decrease incidence of pores and skin most cancers (HR, 0.852; 95% CI, 0.825–0.881; P = 1.00 × 10−9). For most cancers varieties whose incidences have been elevated or decreased by AI-IR, diabetes additionally exhibited an impact in the identical route, whereby in lots of instances, the impact dimension was numerically bigger (Fig. 3 and Supplementary Desk 4).

a Impact of AI-IR and diabetes on the incidence of general and 25 frequent cancers. Cox proportional hazards mannequin was used with a two-sided Wald take a look at. Within the graph, factors signify the estimated HR, and error bars signify 95% confidence intervals. The HRs for indicated cancers, adjusted for age and intercourse have been proven. For male-specific (prostate) or female-specific (uterine and ovary) cancers, HRs have been adjusted just for age. The Bonferroni-corrected P worth for significance was 0.05/43 = 1.163 × 10−3. Supply information are supplied as a Supply information file.
After we outlined composite cancers by merging 10 most cancers varieties (frequent to each women and men) whose dangers have been both considerably elevated (kidney, esophagus, pancreas, colon) or nominally elevated (renal pelvis, small gut, abdomen, liver and GB, colon, and bronchial and lung) by AI-IR, a Kaplan–Meier plot revealed a big distinction between individuals with diabetes, these with out diabetes however constructive for AI-IR, and people with out diabetes and damaging for AI-IR, on the cumulative incidence of the composite cancers (Fig. 4a). The HR adjusted for age and intercourse in individuals with out diabetes however constructive for AI-IR was 1.25 (95% CI, 1.20–1.31; P < 1 × 10−11), and that in individuals with diabetes was 1.40 (95% CI, 1.31–1.50; P < 1 × 10−11). After we adjusted additionally for BMI, the HR in individuals with out diabetes however constructive for AI-IR was 1.16 (95% CI, 1.10–1.22; P = 1.2 × 10−8), suggesting that roughly 36% of AI-IR’ impact is mediated via BMI. Intercourse-specific evaluation revealed that the influence of AI-IR on the incidence of the composite cancers remained constant in each women and men (Supplementary Fig. 3a, b). After we mixed female-specific uterine and breast cancers whose dangers have been considerably elevated by AI-IR, we noticed that impact the HR adjusted for age in individuals with out diabetes however constructive for AI-IR was 1.26 (95% CI, 1.20–1.32; P < 1 × 10−11), which was similar to that in individuals with diabetes (HR, 1.23; 95% CI, 1.11–1.36; P < 3.9 × 10−5) (Fig. 4b). A Kaplan–Meier plot additionally revealed a big distinction between three teams on the cumulative incidence of particular cancers similar to uterine most cancers (Supplementary Fig. 4a), kidney most cancers, colon most cancers, and bronchial and lung most cancers (Supplementary Fig. 4a–d).

a Kaplan–Meier plots of the cumulative incidence of the composite cancers within the DM(-); AI-IR (-), DM(-); AI-IR (+), and DM (+) teams. Within the graph, the strains signify the estimated cumulative incidence, and the shaded error bands signify 95% confidence intervals. The HRs for the incidence of the composite cancers adjusted for age and intercourse or adjusted for age, intercourse, and BMI have been additionally proven. Cox proportional hazards mannequin was used with a two-sided Wald take a look at. b Kaplan–Meier plots of the cumulative incidence of the uterine and breast most cancers in females from the DM(-); AI-IR (-), DM(-); AI-IR (+), and DM (+) teams. Within the graph, the strains signify the estimated cumulative incidence, and the shaded error bands signify 95% confidence intervals. The HRs for the incidence of those cancers adjusted for age or adjusted for age and BMI have been additionally proven. Cox proportional hazards mannequin was used with a two-sided Wald take a look at. c For 13 most cancers varieties whose incidences have been considerably or nominally affected by AI-IR, the results of AI-IR after adjustment for BMI have been proven. Cox proportional hazards mannequin was used with a two-sided Wald take a look at. Within the graph, factors signify the estimated HR, and error bars signify 95% confidence intervals. HRs are adjusted for age and intercourse. The Bonferroni-corrected P worth for significance was 0.05/43 = 1.163 × 10−3. Supply information are supplied as a Supply information file.
Most cancers threat is well-known to extend with age29,30. Certainly, after we stratified individuals by age at enrollment (40–69 years previous), the incidence of the composite cancers per 1000 person-years elevated with age (Supplementary Fig. 5a). Moreover, each AI-IR and diabetes have been related to the next incidence of the composite cancers throughout all ages (Supplementary Fig. 5a), indicating that AI-IR is the danger issue for the composite cancers throughout totally different age teams. Kaplan–Meier analyses additional confirmed constant variations in cumulative incidence of the composite cancers amongst three teams throughout totally different ages at enrollment (<50 years previous, 50–59 years previous, and ≥60 years) (Supplementary Fig. 5b–d). To extra rigorously account for confounding by age, we additionally performed analyses with age because the underlying time variable. Important variations in most cancers incidence continued amongst individuals with diabetes, these with out diabetes however AI-IR constructive, and people with out diabetes and AI-IR damaging (Supplementary Fig. 6a.) The HR adjusted for intercourse and BMI in individuals with out diabetes however AI-IR constructive was 1.16 (95% CI, 1.10–1.22; P < 3.2 × 10−8), and that in individuals with diabetes was 1.29 (95% CI, 1.20–1.39; P < 1 × 10−10). The impact of AI-IR on 3-point MACE was additionally constant in these fashions (Supplementary Fig. 6b). Collectively, these findings reveal the robustness of AI-IR in predicting problems of insulin resistance whereas absolutely accounting for the impact of age.
BMI-dependent and -independent impact of machine learning-predicted insulin resistance on most cancers incidence
In our prediction mannequin, characteristic significance was highest for increased BMI (0.427), adopted by increased FPG (0.115), decrease HDL (0.115), and better TG (0.097)23. To discover the BMI-independent impact of AI-IR on most cancers incidence, we additionally carried out an evaluation adjusted for age, intercourse, and BMI (Fig. 4c and Supplementary Desk 5). Among the many cancers whose dangers have been positively related to AI-IR, we noticed that results for renal pelvis, small gut, abdomen, liver and GB, pancreas, colon, leukemia, and breast most cancers have been BMI-dependent (Fig. 4c). Nevertheless, we noticed that the impact of AI-IR on the incidence of bronchial and lung most cancers grew to become stronger and important even after Bonferroni correction after we adjusted for BMI along with age and intercourse (HR, 1.33; 95% CI, 1.20–1.47; P = 1.71 × 10−8), than after we adjusted just for age and intercourse (HR, 1.14; 95percentCI, 1.05–1.23; P = 2.02 × 10−3) (Fig. 4c), indicating that the impact was unbiased of BMI. The impact on uterine, kidney, and esophagus most cancers remained nominally important. Moreover, the affiliation between AI-IR and decrease threat of pores and skin most cancers was additionally BMI-independent.
Lung most cancers is strongly related to smoking, the main threat issue for the worldwide burden of most cancers31. We noticed that the impact of AI-IR on the incidence of bronchial and lung most cancers is critical even after we adjusted additionally for smoking standing (by no means smoker, earlier smoker, and present smoker); The identical is true for the incidence of the composite cancers (Supplementary Fig. 5a, b). We additionally checked out a doable joint impact of AI-IR and smoking standing on the incidence of bronchial and lung most cancers (Supplementary Fig. 5c). Within the by no means smoker group, HRs adjusted for age, intercourse, and BMI weren’t considerably totally different (P = 0.513) between the AI-IR constructive group (HR, 1.08; 95% CI, 0.85–1.37) and the AI-IR damaging group. Within the present smoker group, HRs adjusted for the three elements have been additionally not considerably totally different (P = 0.726) between the AI-IR constructive group (HR, 17.42; 95% CI, 14.66–20.71) and the AI-IR damaging group (HR, 17.89; 95% CI, 15.63–20.47). However, within the earlier smoker group, HRs adjusted for the three elements within the AI-IR constructive group (HR, 5.52; 95% CI, 4.69–6.49) was considerably increased than that within the AI-IR damaging group (HR, 3.84; 95% CI, 3.35–4.40), when examined by post-hoc evaluation (P = 7.78 × 10−8, Supplementary Fig. 5c). We noticed comparable interplay impact on the incidence of the composite cancers; predicted insulin resistance elevated the incidence within the by no means smoker group and the earlier smoker group, however not within the present smoker group (Supplementary Fig. 5d). Notably, the composite cancers embody esophagus, pancreas, abdomen, liver, and bronchial and lung cancers, all of that are identified to have elevated threat as a result of smoking32. These outcomes recommend that the impact of AI-IR on the incidence of bronchial and lung most cancers or the composite cancers is essentially the most tangible within the earlier smoker group; nevertheless, the impact could have been masked within the present smoker teams as a result of absolutely the dangers of the incidence are overwhelmingly excessive.
Machine learning-predicted insulin resistance permits improved most cancers threat stratification in comparison with beforehand reported metrics
Lastly, to look at whether or not AI-IR gives a greater prediction of the composite most cancers incidence than beforehand established metrics similar to BMI, MetS, TG/HDL ratio, and TyG index, we categorized individuals who have been freed from diabetes and most cancers at baseline into 4 teams in response to their AI-IR standing (constructive or damaging) and the standing of those metrics (constructive or damaging). After we think about AI-IR and BMI, we noticed that the incidence of the composite cancers was considerably increased (P = 2.28 × 10−2) for the AI-IR single-positive group (HR, 1.18; 95% CI, 1.11–1.26; P < 9.5 × 10−8) in contrast with the BMI single-positive group (HR, 1.04; 95% CI, 0.95–1.15; P = 0.38). BMI of 30 or increased alone didn’t considerably enhance the composite most cancers incidence when people have been damaging for AI-IR. We additionally noticed that the incidence of the composite cancers was considerably increased (P = 2.01 × 10−5) within the AI-IR and BMI double-positive group (HR, 1.30; 95% CI 1.24–1.37; P < 1 × 10−11) in contrast with the BMI single constructive group, underscoring that AI-IR gives considerably improved most cancers threat stratification amongst people with weight problems (Fig. 5a). When contemplating AI-IR (constructive or damaging) and MetS (constructive or damaging), the AI-IR single constructive group (HR, 1.21; 95% CI 1.12–1.31; P = 2.1 × 10−6) and the MetS single constructive group (HR, 1.19; 95% CI 1.12–1.26; P = 1.8 × 10−9) exhibited comparable HRs (P = 0.649) for the incidence of the composite cancers. Nevertheless, the incidence of composite cancers was considerably increased (P = 1.49 × 10⁻⁴) within the AI-IR and MetS double-positive group (HR, 1.34; 95% CI 1.27–1.40; P < 1 × 10⁻¹¹) in contrast with the MetS single-positive group (Fig. 5b). Comparable patterns have been noticed after we think about AI-IR and TG/HDL ratio (Fig. 5c). When contemplating AI-IR and TyG index, the incidence of the composite cancers was considerably increased (P = 1.92 × 10−2) for the AI-IR single-positive group (HR, 1.23; 95% CI, 1.13–1.35; P = 7.2 × 10−6) in contrast with the TyG single-positive group (HR, 1.10; 95% CI, 1.05–1.16; P = 1.1 × 10−4). We additionally noticed that the incidence of the composite cancers was considerably increased (P < 1 × 10−11) for the AI-IR and TyG double-positive group (HR, 1.32; 95% CI 1.26–1.39; P < 1 × 10−11) in comparison with the TyG single-positive group (Fig. 5d). Altogether, these outcomes point out that AI-IR permits improved most cancers threat stratification in comparison with beforehand established metrics.

Impact of AI-IR and BMI (a), Metabolic syndrome (MetS) (b), TG/HDL ratio (c), or TyG index (d) on the hazard ratio (HR) for incidence of the composite most cancers throughout the follow-up interval in individuals with out diabetes at baseline. Cox proportional hazards mannequin was used with a two-sided Wald take a look at. Within the graph, factors signify the estimated OR, and error bars signify 95% confidence intervals. Supply information are supplied as a Supply information file.